Abstract
The rising need for structured and efficient blood transfusion services in low-resource settings has driven the adoption of collaborative blood transfusion management systems (CBTMS). This study explores the functionality and impact of the Cornerstone University Blood Management System version 1.0 (CUBMS vs 1.0) in Cameroon. This study was an exploratory research design which used a system interface analysis, comparative case reviews from four countries, and literature synthesis, to reveal that CUBMS improves accessibility, data management, inventory control, emergency responsiveness, and community engagement. Despite infrastructural challenges in rural regions, the system can enhance efficiency, transparency, and safety in blood services. The success of CBTMS in Cameroon is linked to digital infrastructure, training, and culturally relevant community engagement. The Ministry of Public Health of Cameroon should prioritize the nationwide implementation of CBTMS, ensuring consistency in digital health tools.
Author Contributions
Academic Editor: Anubha Bajaj, Consultant Histopathologist, A.B. Diagnostics, Delhi, India
Checked for plagiarism: Yes
Review by: Single-blind
Copyright © 2025 Agwe Lucas Bami, et al
 This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Competing interests
The authors have declared that no competing interests exist.
Citation:
Introduction
The development and implementation of collaborative blood transfusion management systems (CBTMS) have gained global momentum in response to the rising need for structured and efficient blood services. In developed countries like the United Kingdom, the National Health Service Blood and Transplant (NHSBT) has implemented centralized digital inventory management systems that ensure real-time tracking of blood units and reduce wastage 1. Their success is attributed to well-integrated IT platforms, strong government oversight, and public trust in healthcare institutions. In contrast, developing countries face unique constraints. The South African National Blood Service (SANBS) has made commendable progress through mobile blood collection campaigns and educational outreach, significantly improving voluntary blood donation rates in urban centers 2. Similarly, in Malawi, international collaborations with WHO and NGOs have supported the development of rural blood collection units and training programs, contributing to improved blood safety and donor retention 3.
The World Health Organization 4 recommends that national blood systems be based on voluntary, non-remunerated donation, integrated information systems, and consistent quality standards. These components are vital in achieving the goals of universal health coverage and reducing preventable maternal and neonatal deaths. Blood transfusion is a cornerstone of modern healthcare and a vital component in managing surgical procedures, trauma, maternal hemorrhage, anemia, and various hematologic diseases. In Cameroon, access to safe and adequate blood has historically been constrained by structural inefficiencies, insufficient donor pools, and limited laboratory capacity for screening blood, lack of information and inadequate use of ICT tools. The World Health Organization (WHO) recommends that all blood donations be screened for HIV, hepatitis B and C, and syphilis. However, these guidelines are not consistently followed in many parts of Sub-Saharan Africa, including Cameroon, due to resource limitations 5, 6.
In Cameroon, there exist several draw backs to collaborative blood transfusion management system. The absence of a centralized national blood information system means that hospitals and blood banks operate in silos, using different tools that are not interoperable 7, 8. Many rural and peri-urban facilities lack stable internet connectivity and power supply, reducing their ability to use or update ICT systems in real-time 9. Health workers often lack the ICT skills necessary to operate blood management software or analyze digital data. Moreover, training on digital health systems like DHIS2 and BBMIS is often limited to specific projects or pilot hospitals 7. Due to continued reliance on manual documentation in some areas, data entered into digital systems may be incomplete, delayed, or inaccurate. This compromises national reporting and evidence-based planning 8. Current ICT systems do not incorporate advanced capabilities like machine learning for blood demand forecasting, mobile apps for donor location services, or electronic matching algorithms 7. Most tools are basic and used only for recording and reporting. Collaboration between public, private, and nonprofit actors in the blood transfusion chain is limited by the lack of a shared digital communication system or real-time inventory platform 10, 6, 8. More so, Osaro and Charles (2011) emphasize the need for culturally sensitive education campaigns to dispel misconceptions about blood donation, which are widespread in many African contexts.
According to the Cameroon Ministry of Public Health (2017), less than 40% of the annual national demand for blood is met, and most donations come from family members or replacement donors rather than voluntary non-remunerated donors. This reliance on replacement donation increases the risk of transfusion-transmissible infections (TTIs) and delays in emergency response. These findings suggest that the success of CBTMS in Cameroon depends on adapting international best practices to local realities, ensuring community involvement, and building robust digital infrastructure to support timely decision-making and accountability. The CBTMS aims to create a centralized and data-driven approach to ensure efficient blood collection, storage, distribution, and utilization. This paper incorporates the Cornerstone University Blood Management system version 1.0 (CUMBS vs 1.0) to analyze the structure, benefits, and limitations of CBTMS in Cameroon, while drawing parallels to global best practices in blood transfusion management.
Materials and Methods
This study adopted a qualitative design with an exploratory framework to evaluate the functionality, structure, and perceived impact of the Collaborative Blood Transfusion Management System (CBTMS) in Cameroon. The methodology was structured in three phases: system observation and interface analysis, comparative case analysis, and literature synthesis.
Phases of methodology
Phase 1: System Interface Analysis
The CBTMS platform was analyzed through a direct examination of the modules of the Cornerstone University Blood Management System version 1.0 (CUBMS vs 1.0). This comprised of patient registration, donor tracking, hospital data, inventory management, blood bank operations, donation processing, request handling, and transfer logistics. This digital system provided visual insight into each module’s structure and function. These were assessed based on navigational flow, user interface clarity, data entry options, and search and retrieval features. The evaluation focused on how each component enhances efficiency and usability for healthcare workers in both urban and rural settings.
Phase 2: Comparative Case Studies
Best practices from four countries; United Kingdom, Australia, South Africa, and Malawi, were reviewed for comparative benchmarking. These countries were selected due to their innovative approaches in managing blood transfusion systems. Information was sourced from published government reports, academic journals, and World Health Organization (WHO) publications 5, 2, 1, 3. Parameters for comparison included data management capabilities, community involvement strategies, blood safety measures, and integration with broader health systems.
Phase 3: Literature Synthesis
Peer-reviewed studies, WHO guidelines, and national health reports were reviewed to contextualize the CBTMS within global health frameworks 4, 13. The focus was on evaluating how community engagement, digital infrastructure, and training influenced the system’s performance. The synthesis also considered culturally specific factors affecting blood donation in Cameroon and other sub-Saharan countries 10, 11, 12.
Sampling and data sources
This study did not involve human subjects but rather relied on program documentation and interface components as the primary data source. Additional data was drawn from official publications by Cameroon’s Ministry of Public Health, NHSBT (UK), SANBS (South Africa), and the Australian Red Cross. Scholarly articles from PubMed, WHO databases, and the African Journals Online (AJOL) database were also utilized.
Data Analysis Techniques
Content analysis was applied to the user interface modules to identify key themes of efficiency, accessibility, and functionality. A thematic comparison was conducted to map similarities and differences between Cameroon’s CBTMS and international models. Insights were synthesized and validated through triangulation of visual data, published reports, and academic findings. This methodological approach ensured a comprehensive understanding of the CBTMS, providing a strong foundation for evaluating its structure, benefits, and applicability in low-resource settings.
Results and Discussion
The Collaborative Blood Transfusion Management System (CBTMS) in Cameroon has demonstrated substantial improvements in the efficiency, transparency, and safety of blood transfusion services. This section presents the observed outcomes, analyzed according to system modules and corroborated with best practices from comparable international frameworks.
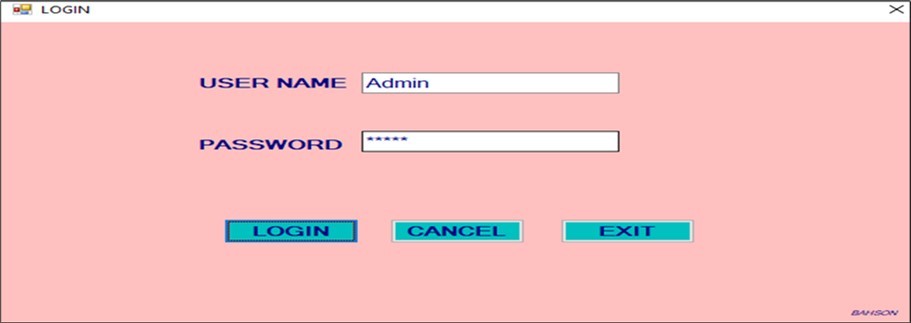
System accessibility and interface usability
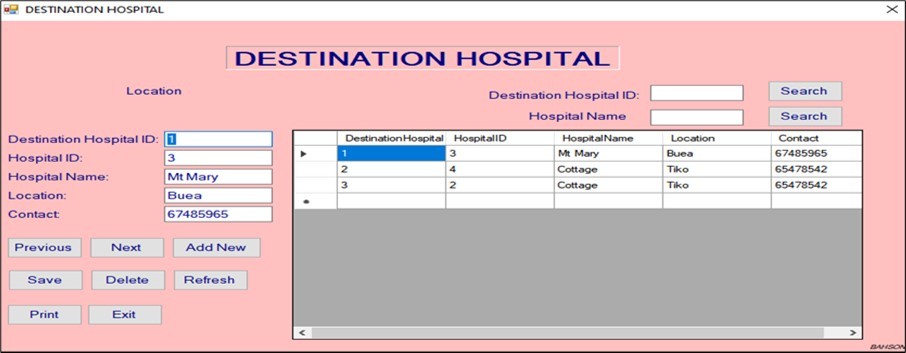
Figure 1 through Figure 2, Figure 3 reveal that the CBTMS provides a user-friendly interface, enabling healthcare professionals with limited IT knowledge to navigate the system effectively. The clear layout of the switchboard interface facilitates access to all operational modules. This aligns with findings by SANBS (2018), where interface simplicity significantly enhanced adoption in peripheral clinics in South Africa.
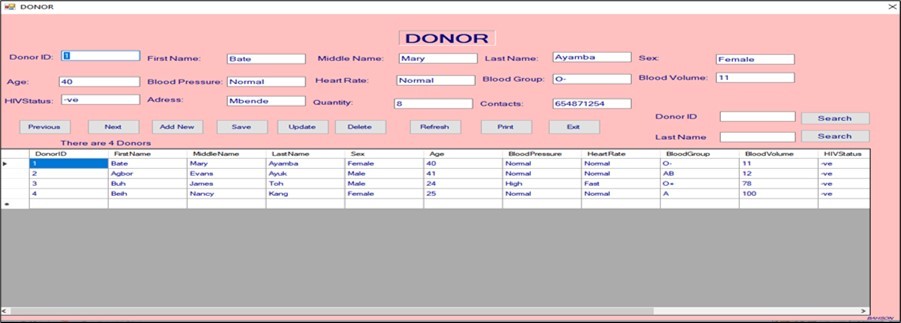
Comprehensive data management
Modules handling patient and donor information (Figure 4 and Figure 5) offer search functions based on patient ID or surname, ensuring quick retrieval and reducing time wasted in emergency settings. The digital recordkeeping allows for cumulative tracking of donor eligibility and blood usage. According to WHO (2017), digital donor records reduce redundancies and contribute to the integrity of blood supply systems.
Figure 4.Patient information window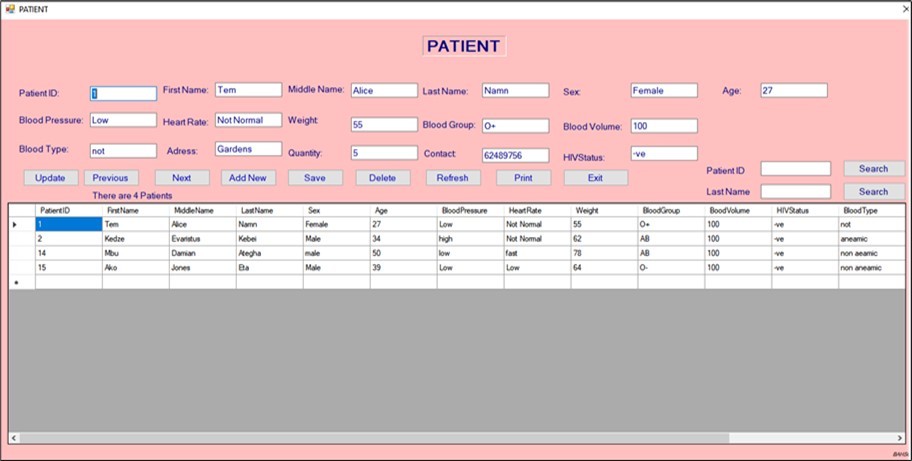
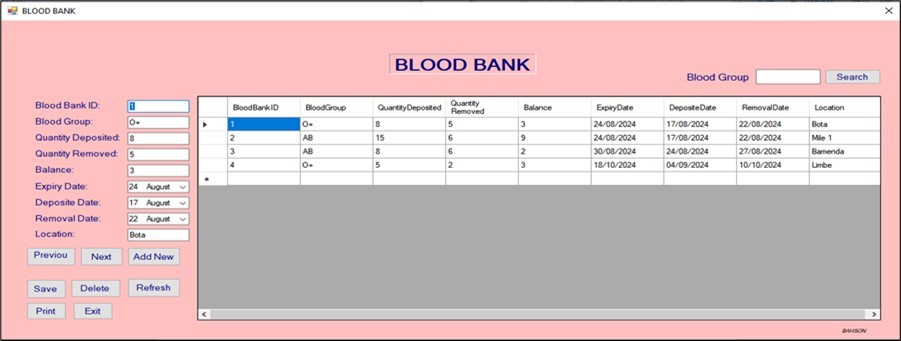
Improved Inventory control and blood safety
Figure 6 to Figure 7, Figure 8 display functionalities for real-time tracking of blood group inventories, unit quantity, and expiration dates. This has minimized shortages and reduced wastage due to expired units. Real-time inventory tracking is consistent with strategies implemented by NHSBT in the UK, which has achieved over 95% blood unit utilization efficiency through centralized digital tracking 1.
Figure 6.Hospital information window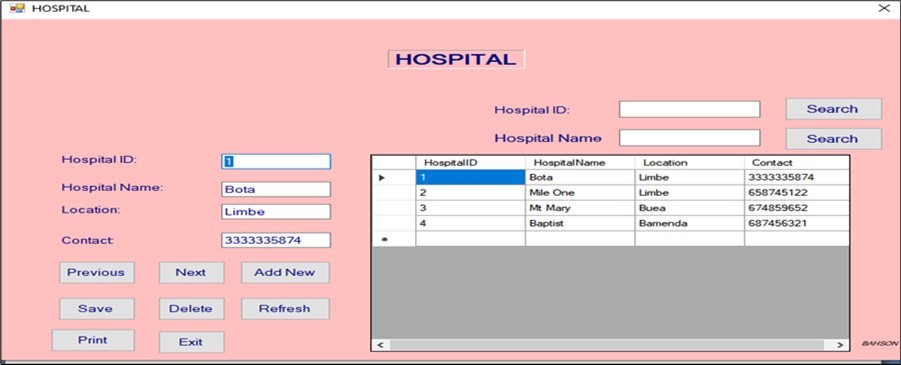
Figure 7.Blood inventory window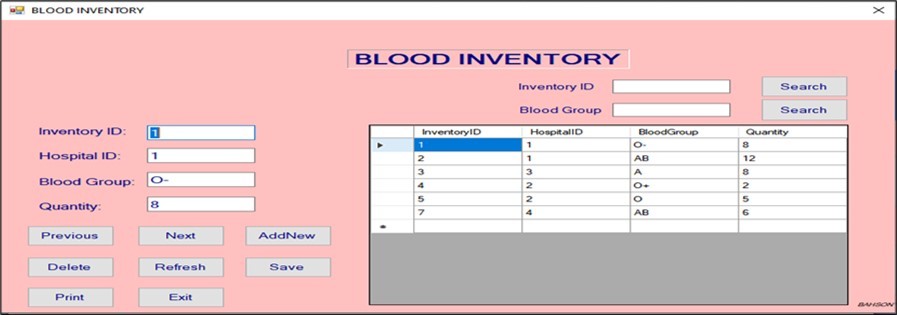
Enhanced emergency response
Modules depicted in Figure 9, Figure 10, Figure 11, Figure 12, Figure 13 support rapid blood requests and transfers between hospitals. In cases where a facility lacks compatible blood, the system allows for immediate routing to another hospital with available stock. This responsiveness is critical in maternal care, trauma, and surgical contexts. A similar emergency transfer model used in Kenya’s Safe Blood for Africa Foundation program reportedly reduced maternal mortality rates by 30% 14.
Figure 9.Blood donation window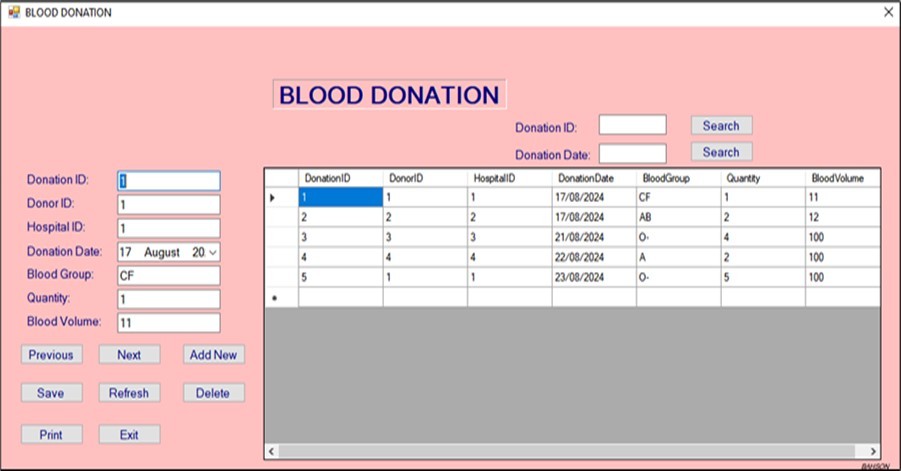
Figure 10.Blood request window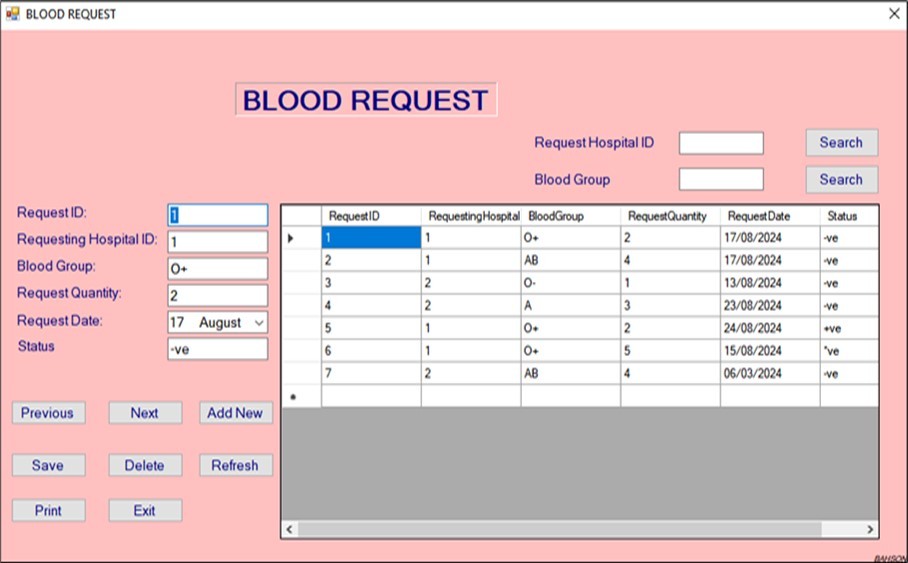
Figure 11.Blood transfer window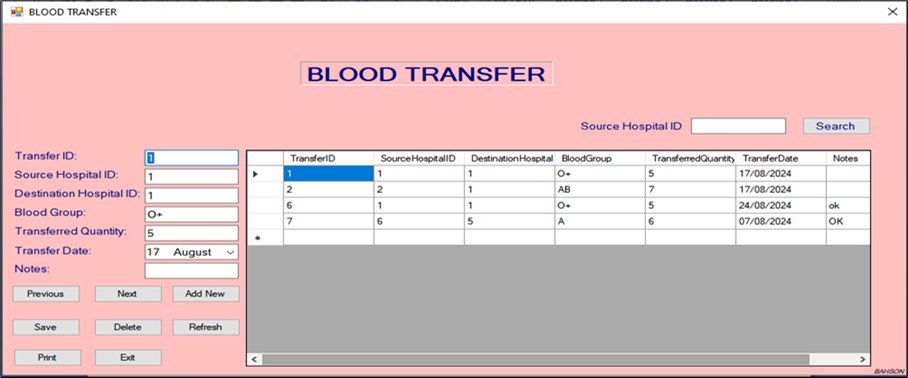
Figure 12.Source hospital window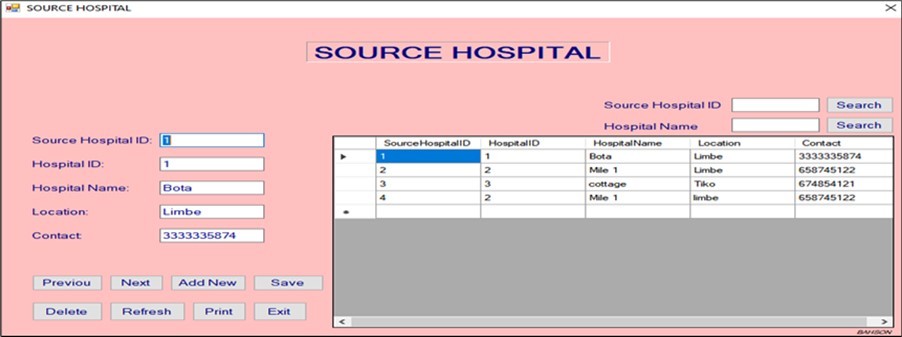
Community engagement and donor mobilization
The CBTMS incorporates community engagement campaigns in collaboration with NGOs and local leaders to raise awareness and recruit voluntary donors. Cultural sensitivities are addressed through education programs aimed at debunking myths and misconceptions about blood donation. Studies by Osaro & Charles (2011) highlight that culturally tailored awareness campaigns significantly increase voluntary donor rates in sub-Saharan Africa.
Capacity building through training
Training programs for healthcare workers have been integrated to improve transfusion practices, reduce administrative errors, and enhance data accuracy. This mirrors the WHO’s recommendations for continuous medical education as a pillar of safe blood transfusion services 5. In Malawi, similar training programs led to a 40% increase in transfusion efficiency 3.
Implementation Challenges
Despite its benefits, the system faces challenges, particularly in rural and underserved regions where internet connectivity is poor. Additionally, reluctance to embrace digital transformation and persistent cultural resistance in certain communities pose obstacles. These issues echo the experiences of early implementation phases in other African contexts, such as in Nigeria, where logistical and cultural challenges slowed program uptake 12.
Conclusions
The Collaborative Blood Transfusion Management System (CBTMS) in Cameroon, exemplified by the Cornerstone University Blood Management System version 1.0, has improved multiple facets of blood transfusion services including digital recordkeeping, inventory control, emergency response, and community engagement. The system offers a sustainable model adaptable to resource-limited settings. However, for its full potential to be realized, challenges related to infrastructure, training, and cultural acceptance must be addressed through coordinated efforts between government, healthcare providers, and community stakeholders.
Recommendations
The Ministry of Public Health should prioritize the nationwide implementation of CBTMS, ensuring consistency in digital health tools.
Continuous training programs should be conducted for healthcare staff to ensure proper utilization of the system.
Investments must be made in ICT infrastructure, particularly in rural areas, to improve system reliability.
Community leaders and NGOs should be engaged to promote voluntary blood donation through culturally sensitive campaigns.
Integration of predictive technologies and AI in future versions of CBTMS can enhance forecasting and supply chain planning.
Author contributions
LBA and HFM conceived, designed, supervised the study and major contributions and performed statistical analysis and drafted manuscript, BEBA participated in designing the projected and carried out data collection in the field. AWC and WDS contributed in the revision of the manuscript. All authors read and approved the final manuscript.
Funding
No special funding was received for this research.
Availability of data and materials
All datasets generated and analyzed during the study are presented in the paper
Ethical Consideration
Not applicable
Acknowledgements
The authors appreciate the Administration of Cornerstone University and Theological Seminary, Cameroon for giving us the opportunity to carry out this project.
References
- 1.J P Allain. (2011) Moving on from voluntary non-remunerated donors: who is the best blood donor?. , British Journal of Hematology 154(6), 763-769.
- 2.GIZ. (2023) Improving Healthcare Infrastructure in Rural Cameroon. Deutsche Gesellschaft für Internationale Zusammenarbeit (GIZ).
- 3.D N Mbanya, J B Tapko, C T Tagny. (2012) Blood safety in Sub-Saharan Africa: a multi-factorial problem. , Transfusion 52(4), 896-902.
- 4.Mbinda A, Kamwendo F, Chinseu E. (2016) Enhancing Blood Transfusion Services through Community Involvement in Malawi. , Malawi Medical Journal 28(2), 78-82.
- 6.NHSBT. (2019) Annual Review: Saving and improving lives. National Health Service Blood and Transplant.
- 7.P A Ndong, B, Tchoumi C. (2020) Evaluating the digital health ecosystem in Cameroon. , Journal of Health Informatics in Developing Countries 14(2), 45-54.
- 8.Osaro E, A T Charles. (2011) The challenges of meeting the blood transfusion requirements in Sub-Saharan Africa. , Asian Journal of Transfusion Science 5(1), 1-2.
- 11.C T Tagny, Mbanya D, J B Tapko, J. (2010) Blood safety in Sub-Saharan Africa: a multi-factorial problem. , Transfusion 50(2), 433-442.